Winning the battle against health care worker injuries, musculoskeletal disorders (MSD), related to mobilizing patients can be agonizing. According to the Bureau of Labor Statistics 2014, health care workers are rated amongst the highest number of reported MSD injuries compared to other industries. Bureau of Labor Statistics (BLS) report in 2014, the frequency of overexertion injuries averaged across all industries was 33 per 10,000 full time workers. By comparison, the overexertion injury frequency for hospital workers was twice the average (68 per 10,000) and the frequency for nursing home workers was over three times the average (107 per 10,000) (NIOSH, 2016). The U.S. Department of Labor’s Occupational Safety and Health Administration (OSHA) has estimated that nearly one half of all healthcare workers will sustain at least one work-related MSD injury in their career and most will be related to a back injury (Converso & Murphy, 2004). The cost of these types of injuries is staggering, “the direct and indirect costs associated with back injuries in the healthcare industry are estimated to be $20 billion annually” (CDC, 2008). To break this down in more relative terms hospitals pay roughly $0.74 per $100 for injury claims. For an average healthcare facility this is a loss of $7,770 per claim with a total approximate cost of $25,450 - $38,280 to replace a nurse after an injury (Harolds & Hurst, 2016).
Safe Patient Handling and Mobility has grown in recognition across the U.S. in the past several years.
Attention has been attributed to the many methods available to mobilize patients through the use of lift equipment, sit to stand devices, slide sheets, air transfer systems, and now more recently facility guidelines for healthcare renovations and construction. These are all very important components to providing a safer environment for both patients and staff. However, there is yet one more gap that may not be considered in many instances and that is the seating surface the patient is transferred to once they are out of bed. Promotion of early progressive mobility is on the forefront of every healthcare institution, or should be, as this promotes a significant cost savings by reducing hospital-acquired conditions (HACs), such as pressure ulcers, pneumonia, urinary tract infections, and deep vein thrombosis to just name a few. Healthcare dollars are very limited and these are challenging times when payer mix is strained and reimbursements for providing care are at an all time low. The cost of pressure ulcers is between $9.1 -11.6 billion per year in the U.S. this impacts approximately 2.5 million patients each year attributing to about 60,000 deaths per year as a direct result of a pressure ulcer (AHRQ, 2014).
The primary point to remember is patients need to get out of bed. As healthcare facilities become very concerned over patient satisfaction the trend is to design the healthcare setting to be very aesthetically pleasing and sometimes this comes at a cost of wasted resources. When selecting patient seating surfaces the bedside clinician must be involved along side the architects and interior designers. If a recliner looks appealing to the color scheme and design of the interior, but it does not promote safe patient transfers the healthcare facility has invested a lot of dollars in recliners that will not be adequately used as it makes it very challenging for patients to egress from low seated chairs; it makes it difficult for healthcare workers to utilize lift equipment and sit to stand devices; and it is ergonomically unfit for the healthcare worker to interact or provide care for the patient when out of bed. Thus resulting in the patient spending more time in bed contributing to the development of HACs. IOA has been very effective as a leader in furniture design identifying safe patient handling needs of both the patient and the healthcare worker. Many healthcare furniture manufacturers have attempted to identify these needs and work them into their designs and have failed, but IOA is the only recliner manufacturer found to have completely addressed the issues aforementioned. IOA has a specific furniture line attributed to safe patient handling.
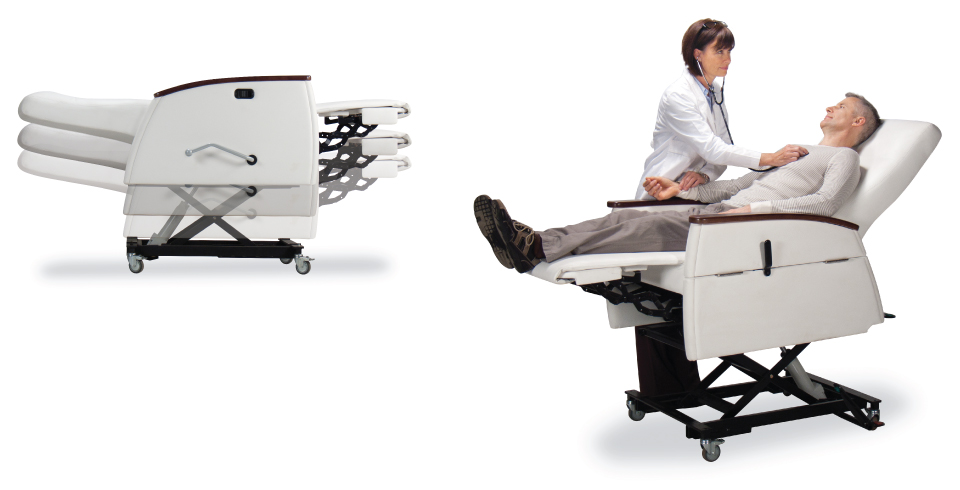
IOA’s Suspend sleeper recliner is designed to accept the arm supports of motorized sit to stand aid between the armrests and castor width to allow the device to achieve a close position to the patient to promote safe transfers. One challenge that was noted with the standard aesthetically pleasing recliners was the low height and angled seat cushion that made it near impossible to utilize our non-motorized sit to stand aid. The staff love this sit to stand frame and were many times unable to use this due to the constraints of the recliner, not the patient mobility status. This can lead to the patient being manually assisted by staff to stand, which can be extremely unsafe and potentially lead to a patient fall or staff injury, or the staff must use a more dependent device such as the ceiling lift to get the patient returned safely to bed. This was challenging because we want to promote early progressive mobility encouraging the patient to provide as much use of his or her own muscle strength as possible. The recliner has been designed with every aspect of patient care considered from a foley bag hook, to a central locking brake, and a fold away arm rest to promote safe transfers and sling placement.
The Connect II Hydraulic recliner is another great recliner that has proven to be very effective from an ICU setting to an outpatient infusion setting. This recliner provides a foot pump to lift the recliner to the height of the bed to provide safe lateral transfers utilizing appropriate safe patient handling devices or to raise the patient to make it easier and safer for them to achieve a standing balance from a seated position. This recliner will also provide opportunities for the nurse starting an IV to elevate the patient to a comfortable work height versus stooping and bending over that can lead to an overexertion injury resulting in days away from work.
These recliners have made a great impact on patient care and staff satisfaction. The staff find them not only aesthetically pleasing, easy to clean, but most importantly another device that can be considered a compliment to their safe patient handling tool box of devices and equipment to provide a more safe working environment for them and ease of mobility for their patients they serve.
Heidi Steenrod, RN, BSN
Patient Advocate Graduate Certificate
Safe Patient Handling Program Coordinator
REFERENCES
Agency for Healthcare Research and Quality. (2014). Are we ready for change?
Agency for Healthcare Research and Quality, Rockville, MD. Retrieved May 1, 2016 from http:www.ahrq.gov/professionals/systems/hospital/pressureulcertoolkit/p uttool1.html
Center for Disease Control. (2008). Preventing back injuries in healthcare settings. NIOSH Science Blog. Retrieved May 1, 2016 from blogs.cdc.gov
Converso, A. and Murphy, C. (2004). Winning the battle against back injuries. United American Nurses, AFL-CIO reprinted from RN February 2004 Advanstar Publication, USA.
Harolds, L. and Hurst, H. (2016). Preventing workplace injuries among perinatal nurses. Nursing for Women’s Health (20) (1) 99-108.
National Institute for Occupational Safety and Health. (2016). Safe Patient Handling. Patient handling hazards. Centers for Disease Control and Prevention Workplace Safety & Health Topics, Atlanta, Georgia. Retrieved May 1, 2016 from CDC.gov
829 Blair Street
Thomasville, NC 27360
fax: 336-476-3016

